
Osteopathy
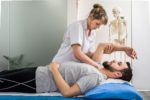 One of the better known forms of complementary medicine, osteopathy detects, treats and prevents a wide variety of medical conditions by moving, stretching and massaging a person’s joints and muscles.
One of the better known forms of complementary medicine, osteopathy detects, treats and prevents a wide variety of medical conditions by moving, stretching and massaging a person’s joints and muscles.
The fundamental principle is that our physical health depends on our bones, muscles, ligaments and connective tissue functioning smoothly together.
Osteopaths use techniques such as massage, stretching and physical manipulation to: increase joint mobility; relieve muscle tension; enhance blood and nerve supply to tissues; and help the body to heal. Advice is provided on posture and exercise to improve health, promote recovery and prevent symptoms returning.
People from a wide range of backgrounds seek osteopathic treatment, from young elite or recreational sports people and pregnant women to manual workers, office professionals and the elderly.
“Osteopaths are well qualified when it comes to identifying the individual needs of those they care for and can adapt the techniques they use to suit the client, young or old,” says Matthew Rogers, head of professional development at the Institute of Osteopathy.
Osteopathy hinges on the theory that the body can repair and defend itself. Problems in one area of the body are thought to affect the rest, so for the body to work well, each element of its structure must function adequately.

Matthew Rogers is head of professional development at the Institute of Osteopathy
Can it help people with osteoarthritis?
Osteopaths use a wide range of gentle hands-on techniques that focus on releasing tension, improving mobility and optimising function. This is often used together with exercise and advice that is designed to help people with arthritis to relieve or manage pain, keep active and maintain health.
Osteopathic treatment does not alter a person’s disease, but it may help reduce side-effects.
There are some situations in which aspects of osteopathic treatment such as manipulation are not suitable (ie if you have osteoporosis or an inflammatory spine condition) but an osteopath should know this and adjust the treatment accordingly.
“Osteopaths as allied health professionals use a wide variety of manual therapy techniques, most of which are gentle movement and stretching based,” explains Matthew. “They are trained to know when each is appropriate and when they are contraindicated. As such, an osteopath would never use a manipulative technique if contraindicated by a patient’s case history.
“A review of the highest level of medical evidence available confirms that there is good evidence that osteopathic care can be effective in the management of arthritic and rheumatic pain, circulatory problems, fibromyalgia, joint pains including hip and knee pain from osteoarthritis as an adjunct to core osteoarthritis treatments and exercise, general, acute and chronic back pain, muscle spasms and neuralgia.”
A spokesperson from Versus Arthritis comments:
“Research into the effectiveness of osteopathy for arthritis remains relatively limited. However, guidance from NICE recommends that manipulation and stretching should be considered alongside core treatments, particularly for osteoarthritis of the hip.
“Osteopathy professionals can play an important role in supporting good musculoskeletal health and many people report the positive impact this treatment has had on their lives. In particular, there is promising evidence to suggest that osteopathy can help to manage lower back pain.
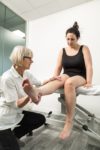 Can it help people with inflammatory arthritis?
Can it help people with inflammatory arthritis?
“Osteopaths may choose not to perform hands-on treatment in an acute flair-up of inflammatory symptoms but can give advice to help people self-manage the associated symptoms,” Matthew highlights.
“When the worst of the symptoms settle down, the osteopath can treat the individual to help to keep them mobile and able to do the things that they want to do. Osteopaths can suggest exercises that can help keep the joints strong, listen to concerns and provide reassurance and support.”
Choosing an osteopath
By law, all osteopaths must be registered with the General Osteopathic Council, which means they have been trained to degree level (four-year master’s course including over 1,000 hours contact time with patients) and have insurance. For additional reassurance, someone who is considering consulting an osteopath should ask if the osteopath is a member of the Institute of Osteopathy, which represents over 70% of the 5,212 osteopaths in the UK and promotes high standards of professionalism.
The appointment
At the start of your first appointment, your osteopath will ask you questions about your medical history and lifestyle, as well as any symptoms you may be experiencing. This helps them to make an accurate diagnosis and suggest appropriate treatment, the likely cost of this and consent to begin treatment.
Most osteopaths will begin your treatment at your first appointment, but sometimes they may require further tests first (such as blood tests or scans). Occasionally they may diagnose an illness that they are unable to treat and may refer you to your GP or another healthcare professional.
Treatment comprises manual therapy, which is a range of gentle hands-on techniques that focus on releasing tension, stretching muscles and mobilising joints.
“The osteopath will need to examine the area(s) of your body causing discomfort,” Matthew says. “Sometimes the cause of the problem may be in a different area to the pain. For example, pain in your lower arm may be linked to the nerves in your neck… so the osteopath may need to examine your whole body. They will need to feel for any tightness in the muscles and stiffness in the joints and may need to touch these areas to identify problems. They will explain what they are doing as they go along.
“If you are uncomfortable with any part of this, you have the right to ask them to stop at any stage, without prejudicing your future treatment.”
You may be given exercises to do at home and advice designed to help you relieve or manage your pain, keep active and maintain the best of health.
What to wear
“As with other healthcare appointments, it may be necessary for your osteopath to ask you to remove some clothing so that they can assess the areas of the body causing you concern,” explains Matthew. “The osteopath will want you to feel at ease, so if you feel uncomfortable undressing to your underwear perhaps wear shorts and a t-shirt, or close-fitting garments that will enable them to work effectively.
“You could choose to seek treatment from an osteopath of the same sex as yourself and/or ask a friend or relative to accompany you and be present throughout your appointment.”
How much does it cost?
Osteopathy is sometimes available on the NHS, but unfortunately it is a bit of a post-code lottery. However, it is readily accessible through private healthcare. On average a first appointment (which includes a healthcare assessment) takes 45–60 minutes and costs around £49. If a follow-up appointment is required (usually about 30 minutes), this will cost about £43. Many healthcare insurance companies do cover osteopathic healthcare.
Is it safe?
“The General Osteopathic Council, whose role it is to regulate the osteopathic profession in the UK to promote patient safety, recently conducted a number of research projects to investigate adverse events associated with osteopathic practice,” says Matthew. “Following these research projects, which included a review of published literature to investigate the risks associated with manual therapy it was determined that: ‘Osteopathy has an extremely safe reputation and a major adverse event occurrence is very rare, rarer than for taking medication’.”
Osteopathic treatment is usually a very gentle process and osteopaths work hard to make treatment as painless as possible. You may, however, experience some discomfort during and after treatment. Your osteopath will warn you if they think that the technique that they are about to use is likely to be uncomfortable and will stop if you tell them that you are feeling too much pain.
Following treatment, you may experience some mild soreness in the area of the body that was treated, which normally resolves within 48 hours. If you experience serious or unusual symptoms after treatment, you should contact your osteopath straight away for advice.
The bottom line
Osteopathy can help reduce some symptoms of arthritis. Aspects of osteopathic treatment such as physical manipulation are not suitable in certain situations but an osteopath should know this and adjust the treatment accordingly. Make sure that your osteopath is registered with the General Osteopathic Council and ideally the Institute of Osteopathy.
Further information:
- The General Osteopathic Council, visit osteopathy.org.uk or tel 020 7357 6655
- The Institute of Osteopathy, visit iosteopathy.org or tel 01582 488 455
True story: Alison Newman, aged 59 from Cornwall
“I was diagnosed with osteoarthritis about 15 years ago and then with polymyalgia rheumatica just over a year ago. The latter causes pain, stiffness and inflammation in the muscles around the shoulders, neck and hips.
“I currently take paracetamol and a nonsteroidal anti-inflammatory drug called naproxen that relieves pain, swelling, and stiffness of osteoarthritis; codeine phosphate (to manage the pain of osteoporosis); and steroids (to reduce symptoms of polymyalgia rheumatic).
“I first visited an osteopath just over a year ago after being recommended by a friend. My biggest problem has been the restricted movement in my neck area, but regular osteopathy visits have improved the movement. Beforehand I had to use my car mirrors for reversing as I was unable to move my neck enough whereas I now have a much better range of movement.
“Initially I had to visit the osteopath a couple of times a month and the first visits left me in pain which wore off after a couple of days. Now I only need to visit every three months and although I am a little sore afterwards, this soon wears off.
“I would encourage anyone suffering to take the plunge and visit an osteopath. They treat the whole body and while you come away feeling sore, this wears off and the treatment really helps in the long run.”
